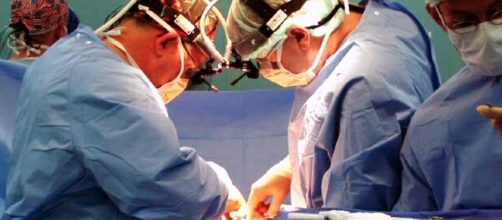
It is not a secret that organ transplants save lives. Unfortunately, a patient's body often rejects their new organ, causing them to need another transplant. Researchers at the University of Pittsburgh (Pitt) believe they have identified the cause of organ rejection.
Over 50% of transplant organs are rejected
Organ rejection occurs when the patient's Immune System recognizes the new organ as a threat and initiates an attack against it. Cancers and other biological toxins have proteins known as antigens on the surface of their cells. All cells have proteins which allow them to be recognized by neighboring cells.
When an organ is rejected, the body has recognized its proteins as antigens. This, in turn, causes an immune reaction which leads to rejection of the organ. Organ rejection can lead to fever, nausea, difficulty breathing, and swelling of the organ and surrounding tissues.
In order to avoid rejection, physicians go through an extensive matching process to make sure the donor organ is as similar to the patient's as possible. Despite best efforts, this is not always enough to guarantee that the organ will not be rejected. In order to further reduce the risk, patients are given a medication that prevents the new organ from activating the immune system. This drug is not 100% effective and has some serious side effects.
These drugs weaken the immune system in an attempt to prevent rejection, but this also makes the recipient more susceptible to illnesses. Additionally, they can increase the risk or cancer, heart attacks, and stroke.
Even with these medications, 50% of organs are rejected within a decade of the transplant.
Pitt scientists build on current knowledge of the immune system to understand organ rejection
Researchers at the Thomas E. Starzl Transplant Institute at the University of Pittsburgh partnered with scientists at the University of Toronto with the goal of examining the causes of organ rejection. The first step was an investigation into the human immune system. The immune system consists of organs such as the lymph nodes and the spleen that help the body to fight off disease.
It can be split up into two major parts: the innate immune system and the adaptive immune system. The innate immune system is not specific to the pathogen. When it is activated, it creates responses that release chemicals into the blood and send out immune cells to fight the infection. The adaptive immune system is specific to the antigen. With an adaptive immune response, the antigen must be identified before creating immune cells that are designed to be able to kill that pathogen.
Previous research already identified the adaptive immune system's role in organ rejection. However, scientists were unsure about what caused the activation of the adaptive immune system in the first place. The adaptive immune system is activated in response to a signal made by the innate immune system.
The innate immune system must be initiated in order for the adaptive immune system to be activated. Pitt researchers set out to discover what it is about organ transplants that cause the innate immune system to become activated.
Scientists performed organ transplants on mice and found a protein called SIRP-alpha which binds to the surface of white blood cells. Once this protein attached itself to the white blood cells, the innate immune system became activated. In response to the activation of the innate immune system, the adaptive immune system was activated, which ultimately caused the organ to be rejected.
It is believed that differences in the SIRP-alpha protein between the original organ and the donor organ cause the immune system to become activated.
Proteins vary from person to person. If the donor had a slightly different version of the SIRP-alpha protein then the recipient, the immune system would likely recognize it as a foreign invader and thus attack.
Fadi Lakkis, the scientific director of the Thomas E. Starzl Transportation Institute, says the next step for his team is to conduct a full genetic sequence of the SIRP-alpha protein in a variety of donors and recipients. They will be looking to see if variations in this protein are linked to a higher rate of organ rejection. If scientists are able to prove that better SIRP-alpha matches lead to fewer organ rejections, it could completely change the way organ transplants are handled. People would be able to receive organs that were better matches, and as a result would be able to take smaller doses of the anti-rejection medications.